Did you know that nearly 32% of the global adult population now lives with a condition formerly known as nonalcoholic fatty liver disease? This silent epidemic is being redefined as MASLD (Metabolic Dysfunction-Associated Steatotic Liver Disease) to reflect its true metabolic origins. If you’re feeling overwhelmed by new medical jargon or the fear of irreversible scarring, you’re not alone in this journey.
It’s frustrating to receive vague advice like "eat better" when you’re looking for a concrete clinical roadmap to protect your health. We understand that you want to move beyond the confusion of MASH and MASLD toward tangible results and faster recovery. You deserve a plan that prioritizes your long-term well-being over generic suggestions.
This article promises to help you discover how to identify, monitor, and reverse liver fat through a modern, integrated metabolic approach. We’ll preview the latest medical advancements, including the March 14, 2024, FDA approval of resmetirom, and explain how non-invasive tools like FibroScan provide a clear picture of your liver health without the need for painful biopsies. Gain the clarity you need to fast-track your path to a healthier liver today.
Key Takeaways
- Understand why fatty liver is now clinically defined as MASLD and how this metabolic shift refocuses your treatment on long-term health.
- Identify the specific stages of liver progression to recognize when simple fat transitions into dangerous inflammation known as MASH.
- Gain immediate clarity on your liver health through non-invasive “Fast-Track” diagnostics like Fibroscan that measure stiffness without a biopsy.
- Discover how bespoke medical weight management and metabolic testing provide a clinical roadmap to actively reverse liver damage.
- Learn the benefits of an integrated, multi-disciplinary approach that handles all your digestive needs under one roof for a faster recovery.
Table of Contents
-
Understanding Fatty Liver: Why MASLD is the "Silent" Epidemic
-
The Progression Spectrum: From Simple Fat to MASH and Cirrhosis
-
Fast-Track Diagnosis and Reversal: Fibroscan and Metabolic Testing
-
Comprehensive Liver Care: Reversing Fatty Liver Under One Roof
Understanding Fatty Liver: Why MASLD is the "Silent" Epidemic
The global health landscape is shifting. Recent data from May 2026 indicates that Fatty Liver Disease (FLD) now affects approximately 32% of the adult population worldwide. In Singapore, this condition has become a primary focus for metabolic health specialists because it often progresses without a single outward symptom. Many patients only discover they have fatty liver during routine health screenings or when investigating unrelated digestive issues. This lack of early warning signs is why clinicians refer to it as a "silent" epidemic; by the time symptoms like jaundice or intense fatigue appear, the liver may already face significant damage.
As a modern specialist healer, our approach moves beyond simply identifying the illness. We focus on proactive metabolic health to prevent the transition from simple fat accumulation to advanced scarring. Understanding your liver’s current state is the first step toward gaining health and ensuring a faster recovery through an integrated, medical roadmap.
The Shift from NAFLD to MASLD
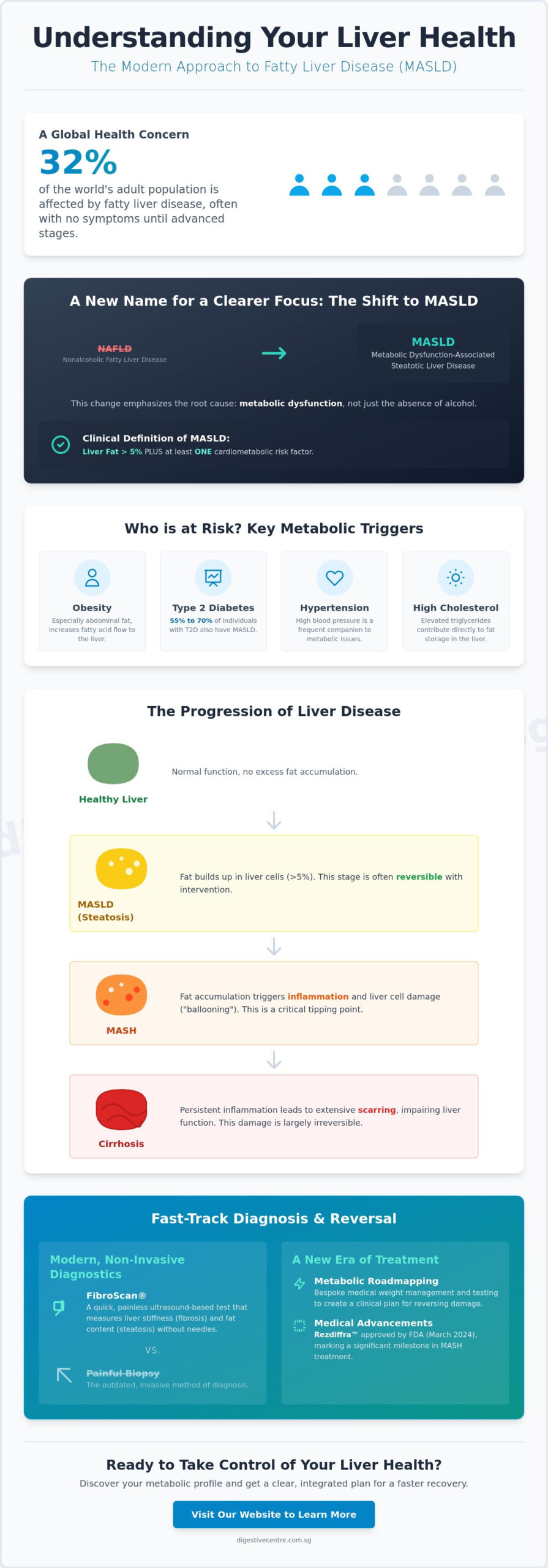
In mid-2023, a global consensus panel officially renamed Nonalcoholic Fatty Liver Disease (NAFLD) to Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD). This 2026 terminology shift isn’t just a name change; it’s a fundamental pivot toward addressing the root cause: metabolic dysfunction. By focusing on how the body processes energy and insulin, doctors can better tailor treatments to your specific biology. Under these modern guidelines, MASLD is clinically defined as a condition where liver fat exceeds 5% of the total organ weight combined with at least one cardiometabolic risk factor.
Who is at Risk? Identifying the Metabolic Triggers
The triggers for liver fat accumulation are closely tied to how our bodies manage sugar and fats. While lifestyle choices play a role, your metabolic profile is the primary driver. The most common risk factors include:
-
Obesity: Excess body fat, particularly around the abdomen, increases the flow of fatty acids to the liver.
-
Type 2 Diabetes: An estimated 55% to 70% of individuals with type 2 diabetes also live with MASLD.
-
High Blood Pressure: Hypertension is a frequent companion to metabolic liver issues.
-
High Cholesterol: Elevated levels of triglycerides directly contribute to fat storage in liver cells.
It’s a common misconception that only those with a high Body Mass Index (BMI) are at risk. Even "lean" individuals can develop metabolic liver issues if they possess high visceral fat or genetic predispositions to insulin resistance. This makes comprehensive metabolic testing essential for everyone, regardless of their appearance on a scale. Our goal is to provide you with a bespoke plan that addresses these triggers before they lead to permanent complications.
The Progression Spectrum: From Simple Fat to MASH and Cirrhosis
Liver health doesn’t deteriorate overnight. It’s a progressive journey that often begins with simple steatosis, a stage where fat accumulates within liver cells but hasn’t yet caused significant inflammation. While this early stage might feel harmless, it’s the critical window where intervention is most effective. Historically, this was categorized under Nonalcoholic Fatty Liver Disease (NAFLD), but we now understand that this fat accumulation is a metabolic warning light. If left unmanaged, the liver can transition from storing fat to a state of active injury.
The good news is that early-stage fatty liver is often reversible. By utilizing an integrated metabolic approach, we can halt the progression before the organ reaches the point of no return. Our goal is to move you toward a faster recovery by identifying exactly where you sit on the spectrum through precise diagnostic tools.
What is MASH (Steatohepatitis)?
Metabolic Dysfunction-Associated Steatohepatitis, or MASH, represents the aggressive "tipping point" of liver disease. At this stage, the fat in your liver triggers a cascade of inflammation and cellular damage. Doctors look for "ballooning," a process where liver cells swell and eventually die. This chronic injury is a medical emergency because it signals that the liver’s natural repair mechanisms are being overwhelmed. Globally, MASH has become a leading cause for liver transplants, yet many patients remain unaware of the danger because the inflammation doesn’t always cause physical pain. Transitioning from simple fat to MASH increases the risk of developing liver cancer or cardiovascular complications significantly.
The High Cost of Delay: Understanding Fibrosis
When inflammation persists, the liver attempts to heal itself by creating scar tissue. This process is known as fibrosis. Unlike healthy liver tissue, which is soft and flexible, fibrotic tissue is stiff and dysfunctional. As scarring increases, it restricts blood flow and impairs the liver’s ability to detoxify your body and regulate metabolism. If this scarring becomes widespread, it leads to cirrhosis, a late-stage condition that is much harder to treat.
The latest clinical guidelines from May 2026 emphasize a fibrosis-centered approach to risk stratification. We prioritize identifying these scars early using non-invasive technology like FibroScan to ensure you don’t reach the stage of irreversible damage. Proactive screening is the most reliable way to avoid the complications of advanced disease. If you’re concerned about your liver health, you can schedule a comprehensive metabolic assessment to get a clear clinical roadmap for your recovery.
By intervening during the MASH or early fibrosis stages, we can often achieve a reduction in liver fat and even a regression of scar tissue. Modern pharmacotherapies, such as resmetirom which received accelerated FDA approval on March 14, 2024, are now providing new hope for patients with moderate to advanced fibrosis. This new era of treatment means that a fatty liver diagnosis is no longer a life sentence, provided you take action with a specialist who understands the metabolic "how" and "why" behind your condition.
Beyond Alcohol: Debunking Common Myths About Liver Fat
Many patients arrive at our clinic surprised by their diagnosis. They often believe that liver damage is reserved for those who consume excessive alcohol. While Alcohol-associated Liver Disease (ALD) is a distinct condition, Metabolic Dysfunction-Associated Steatotic Liver Disease (MASLD) is driven by metabolic factors rather than the bottle. This distinction is crucial for your recovery. As your caring advisors, we look beyond lifestyle stereotypes to understand the unique biological drivers of your fatty liver.
One of the biggest hurdles to treatment is the "I feel fine" objection. Because the liver has few pain receptors, you won’t feel the fat accumulating or the early stages of inflammation. Waiting for physical symptoms often means waiting for the disease to reach an advanced stage. By taking a proactive approach now, you’re choosing a path of less pain and shorter downtime in the future.
Myth 1: "I Don’t Drink, So My Liver is Fine"
Your liver processes everything you eat and drink. In a modern diet rich in processed carbohydrates and high-fructose corn syrup, the organ can become overwhelmed even without a drop of alcohol. When you consume excess calories, your liver converts them into hepatic triglycerides through a process called de novo lipogenesis. This means that sugary drinks, white rice, and refined snacks can be just as damaging to liver cells as spirits. MASLD is the most common liver disorder worldwide, affecting approximately 32% of adults regardless of their alcohol consumption levels. Understanding this helps you focus on the right metabolic targets for a faster recovery.
Myth 2: "Fatty Liver is Just a Cosmetic Issue"
It’s easy to dismiss a "slightly fatty" liver as a minor consequence of weight gain. However, liver fat isn’t inert storage; it functions like a "toxic factory" that releases inflammatory markers into your bloodstream. This systemic inflammation increases your risk of developing cardiovascular disease, which remains the leading cause of mortality for those with metabolic liver issues. Monitoring the progression of fatty liver disease is vital because it protects your heart as much as your digestive system.
Gaining health is about more than just aesthetics. By treating the liver, you improve your body’s ability to regulate blood sugar and cholesterol, leading to higher energy levels and a lower risk of chronic illness. We provide the clinical tools and support needed to turn this "silent" issue into a proactive health victory. You don’t have to wait for symptoms to appear to take control. Early intervention ensures that your path to recovery is handled with professional speed and minimal friction. Our multi-disciplinary approach ensures all your metabolic needs are met under one roof. Patients managing metabolic conditions should also be aware that digestive symptoms such as blood in the stool warrant prompt evaluation; understanding the rectal bleeding causes Singapore specialists prioritize can help you act quickly and avoid delayed diagnoses.
Fast-Track Diagnosis and Reversal: Fibroscan and Metabolic Testing
Clarity is the foundation of confidence. Our Fast-Track diagnostic philosophy is designed to eliminate the anxiety of the unknown by providing a comprehensive assessment of your liver health in a single, efficient visit. While many general practices rely on standard blood tests that may only flag issues once damage is advanced, we utilize high-precision tools to detect fatty liver at its earliest, most reversible stages. This proactive approach ensures you spend less time worrying and more time on a clear path to recovery.
A personalized screening goes far beyond a generic "check-up." By integrating advanced imaging with detailed metabolic analysis, we create a bespoke roadmap tailored to your body’s specific needs. This level of detail allows us to identify the "why" behind your liver fat accumulation, whether it’s driven by insulin resistance, lipid imbalances, or nutritional gaps. You deserve a diagnostic process that is as sophisticated as the treatment that follows.
The Power of Fibroscan: No Needles, No Pain
In the past, confirming the stage of liver disease often required an invasive biopsy. Today, we offer Fibroscan technology, a non-invasive ultrasound-based tool that provides immediate results with zero downtime. This "Modern Specialist Healer" approach prioritizes your physical comfort, delivering the same essential data as a biopsy without the need for needles or hospital stays. The procedure takes approximately 10 minutes and allows you to return to your daily activities immediately.
Fibroscan provides two critical measurements: the CAP score and the E-score. The CAP score quantifies the exact percentage of fat in your liver, while the E-score measures liver stiffness in kilopascals (kPa). These numbers are vital for tracking your progress; as you follow your reversal plan, you’ll see these values decrease, providing tangible proof that you’re gaining health. Every metabolic assessment we perform includes this assessment to ensure no detail of your liver’s condition is overlooked.
Integrated Metabolic Testing
Effective reversal requires looking at the body as a whole. Our integrated metabolic testing evaluates your insulin sensitivity through markers like HOMA-IR and examines your full lipid profile to understand how your body processes fats. We don’t just look at whether your liver enzymes are "within range"; we look for optimal metabolic function. This data-driven strategy allows us to move beyond vague lifestyle advice and provide clinical interventions that work.
Nutritional counseling acts as a pillar of this journey. Once we understand your metabolic triggers, our team provides a personalised plan to reduce hepatic triglycerides and improve your energy levels. This comprehensive method ensures all your digestive and metabolic needs are handled under one roof. If you’re ready to stop guessing and start healing, you can book a Fast-Track liver screening to receive your clinical roadmap today. By intervening now, you’re choosing a future with less pain and a significantly faster recovery.
Comprehensive Liver Care: Reversing Fatty Liver Under One Roof
Reversing a fatty liver diagnosis requires more than just a suggestion to "exercise more." It demands a clinical roadmap that addresses the metabolic root causes of your condition. As a Modern Specialist Healer, our center provides a sophisticated environment where medical authority meets empathetic care. We focus on the positive outcomes of your treatment, ensuring that every step of your journey is designed for gaining health and achieving a faster recovery. By housing diagnostics, specialist consultations, and advanced treatments in one location, we ensure all your digestive needs are handled under one roof with professional speed.
Traditional advice often leaves patients frustrated with vague goals. We replace that confusion with an integrated approach that utilizes the latest medical advancements. Whether your condition is in the early stages of MASLD or has progressed to MASH, our multi-disciplinary team provides the specific clinical tools necessary to halt and reverse liver damage. You don’t have to navigate this complex metabolic journey alone.
Medical Weight Loss: GLP-1s and Liver Health
In August 2025, the medical community saw a significant breakthrough with the FDA approval of semaglutide for treating MASH in adults with moderate to advanced liver fibrosis. These modern weight loss medications do more than just reduce numbers on a scale; they target the metabolic dysfunction that drives liver fat accumulation. By improving insulin sensitivity and reducing systemic inflammation, GLP-1 receptor agonists help your liver cells recover and regenerate. This clinical weight control is a powerful tool for those who have struggled with traditional methods, providing a reliable path toward less pain and shorter downtime in your health journey.
Advanced Interventions: ESG and Bariatric Options
When lifestyle changes and medications aren’t enough to achieve the necessary metabolic shift, we offer advanced endoscopic interventions. Endoscopic Sleeve Gastroplasty (ESG) is a non-surgical procedure that reduces stomach capacity without the need for external incisions or permanent scars. This technique significantly improves metabolic markers and liver enzymes, often leading to a rapid reduction in hepatic fat. Because ESG is performed endoscopically, patients benefit from our core promise of less pain and a faster return to daily life. Our holistic journey combines these cutting-edge procedures with bespoke nutritional support to ensure your results are sustainable. Patients who experience persistent bowel changes alongside their metabolic condition should also consider that colonoscopy for bowel problems in Singapore remains the most definitive diagnostic tool for evaluating chronic digestive symptoms with both accuracy and therapeutic value.
Your Path to Gaining Health
Choosing a proactive path today prevents the risk of irreversible scarring tomorrow. Our integrated approach ensures that your treatment is personalized to your unique metabolic profile, giving you the best possible chance for a full reversal. From your initial Fast-Track screening to advanced medical or endoscopic interventions, we handle every detail with professional efficiency and care. We invite you to take the first step toward a healthier future by securing a clinical assessment of your liver health. Book your liver health assessment at Digestive Centre and discover a comprehensive roadmap tailored to your recovery.
Take Control of Your Metabolic Health Today
A diagnosis of fatty liver is a significant metabolic warning, but it’s also a clear opportunity to pivot toward a healthier future. You now understand that MASLD is a treatable condition when addressed with a clinical roadmap rather than vague lifestyle advice. By utilizing non-invasive tools like FibroScan and advanced metabolic testing, you can achieve immediate clarity on your liver’s health without the need for painful biopsies.
Led by Senior Consultant Surgeon Dr. Shanker Pasupathy, Digestive Centre provides a comprehensive environment where all your digestive needs are handled under one roof. Our Fast-Track diagnostic programs deliver immediate results, allowing us to implement bespoke strategies like medical weight management or ESG with professional speed. We promise less pain, shorter downtime, and a faster recovery as you move toward gaining health. Don’t wait for silent inflammation to progress into permanent scarring. You can start your liver reversal journey today with a partner who prioritizes your long-term well-being. Your path to a restored liver and improved vitality begins with a single, proactive step.
Frequently Asked Questions
Can fatty liver be reversed completely?
Yes, fatty liver is often completely reversible if you intervene during the early stages of fat accumulation. By following a clinical roadmap that includes metabolic testing and targeted weight management, you can reduce hepatic fat and even resolve early-stage inflammation. Once the condition progresses to advanced cirrhosis, reversal becomes much more difficult, which is why early screening is essential for a faster recovery.
What are the early warning signs of fatty liver disease?
Most individuals experience no symptoms at all during the early stages of liver fat accumulation. It’s estimated that 32% of the global adult population lives with this condition silently. Some patients report mild fatigue or a dull ache in the upper right side of the abdomen, but these signs are rare. You shouldn’t wait for physical symptoms to appear before seeking a professional metabolic assessment.
Is there a specific medication to cure fatty liver?
The FDA granted accelerated approval to resmetirom on March 14, 2024, making it the first medication specifically approved for MASH with moderate to advanced fibrosis. Additionally, medications like semaglutide received FDA approval in August 2025 to help manage the metabolic drivers of the disease. These pharmacological interventions work most effectively when integrated into a comprehensive, multi-disciplinary care plan under specialist supervision.
How does a Fibroscan differ from a regular ultrasound?
A Fibroscan uses vibration-controlled transient elastography (VCTE) to measure liver stiffness and fat percentage, providing numerical data that a standard ultrasound cannot. While a regular ultrasound only offers a visual image of the organ, Fibroscan delivers a CAP score for fat and an E-score for scarring. This allows our specialists to track your progress with high precision and provide immediate results during your consultation.
What foods should I avoid if I have MASLD?
You should prioritize avoiding high-fructose corn syrup, sugary beverages, and refined carbohydrates like white rice and white bread. These foods trigger de novo lipogenesis, a process where the liver converts excess sugar directly into fat. Reducing your intake of trans fats and processed snacks is also vital for lowering systemic inflammation and supporting the long-term health of your liver cells.
How much weight do I need to lose to improve my liver health?
Losing 5% to 7% of your total body weight is often enough to reduce fatty liver accumulation significantly. If your goal is to reverse active inflammation or improve fibrosis, clinical guidelines typically recommend a weight loss target of 10% or more. Utilizing medical tools like GLP-1 medications or Endoscopic Sleeve Gastroplasty (ESG) can help you reach these targets with less pain and more consistency.
Is fatty liver disease hereditary?
Genetic factors can increase your susceptibility, but they aren’t the sole cause of the condition. Variants in genes like PNPLA3 can make your liver more likely to store fat, even if you don’t have a high BMI. However, your metabolic profile and lifestyle choices remain the primary drivers of disease progression. If you have a family history of liver issues, a proactive Fast-Track screening is highly recommended.
What happens if I leave fatty liver untreated?
Neglecting treatment can lead to Metabolic Dysfunction-Associated Steatohepatitis (MASH), which causes chronic inflammation and irreversible scarring known as cirrhosis. Over time, this scarring impairs the liver’s ability to detoxify your blood and can eventually lead to liver failure or liver cancer. Furthermore, individuals with untreated MASLD face a significantly higher risk of cardiovascular disease, which remains the leading cause of mortality for this group. As part of a comprehensive digestive health strategy, it is equally important to investigate any new bowel symptoms promptly; a specialist guide to rectal bleeding causes in Singapore can help you understand when to seek urgent evaluation alongside your liver care.

