Over 50.8% of people in developing nations currently live with the stomach inflammation known as gastritis. In Singapore, it’s common to dismiss a persistent, gnawing ache as simple indigestion or “gastric pain” caused by a hectic schedule. You might feel anxious about whether your discomfort requires a diagnostic gastroscopy or if it’s something you can manage alone. It’s normal to feel confused when trying to distinguish between a temporary upset and a condition that needs specialist intervention for your gastritis symptoms.
We’re here to provide a clear roadmap to a pain-free digestive system. You’ll learn how to recognise the early warning signs and the professional steps required for a faster, pain-free recovery. This guide explores the difference between acute and chronic inflammation, the importance of a fast-track diagnosis, and how bespoke, integrated care can help you gain health with less pain and shorter downtime. At our centre, we bring all your digestive needs under one roof to ensure your journey to wellness is efficient and supportive.
Key Takeaways
- Identify the specific “gnawing” or “burning” sensations in the upper abdomen that distinguish gastritis symptoms from standard indigestion.
- Understand the critical differences between sudden, severe acute gastritis and the silent, long-term risks associated with chronic inflammation.
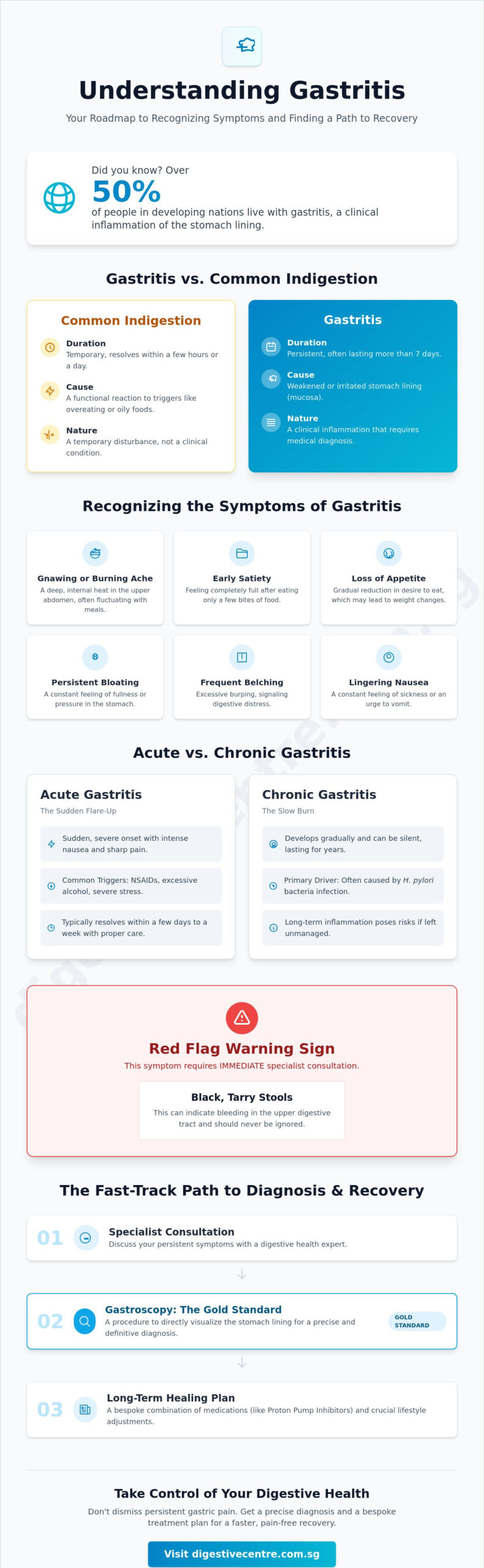
- Learn to recognise urgent “red flag” warning signs, such as black, tarry stools; these necessitate an immediate specialist consultation.
- Discover why a gastroscopy is considered the gold standard for a precise diagnosis and a “fast-track” path to a pain-free recovery.
- Establish a roadmap for long-term healing using a combination of generic medications like proton pump inhibitors and bespoke lifestyle adjustments.
Recognising the Common Symptoms of Gastritis
Gastritis is the clinical inflammation of the protective stomach lining, known as the mucosa. This lining is responsible for shielding your stomach wall from the highly acidic juices required for digestion. When this barrier weakens or becomes irritated, the resulting inflammation triggers a range of physical signals. While many people in Singapore experience occasional “gastric” pain after a spicy meal, true gastritis symptoms are often more persistent and indicative of an underlying issue that requires professional attention. Identifying these signs early is the first step toward a faster recovery and gaining health.
Sensory Indicators: What Gastritis Feels Like
The most frequent sensation associated with this condition is a gnawing or burning ache in the upper abdomen, specifically the epigastrium. Unlike the sharp, stabbing pain of a muscle strain, this discomfort often feels like a deep, internal heat. For some, the pain behaves like a dull, constant background ache that never quite disappears. These sensations frequently fluctuate based on meal timing; some individuals find relief after eating, while others experience a significant spike in discomfort as soon as they finish a meal.
Another hallmark indicator is early satiety. This occurs when you feel completely full after consuming only a few bites of food, even if you were hungry moments before. This often leads to a “hidden” symptom: a gradual loss of appetite. When eating becomes associated with discomfort, patients naturally consume less, which can lead to unintentional weight changes. Secondary symptoms like persistent bloating, frequent belching, and a lingering sense of nausea also suggest that the stomach lining is struggling to manage normal digestive processes.
Gastritis vs. Common Indigestion
It is easy to confuse gastritis with simple indigestion, but the two differ significantly in duration and cause. Indigestion, or dyspepsia, is typically a temporary reaction to specific triggers like overeating or consuming oily foods. It usually resolves within a few hours or a day. In contrast, gastritis symptoms are remarkably persistent, often lasting for more than seven days regardless of what you eat.
While indigestion is a functional disturbance, gastritis is a clinical inflammation of the mucosa that requires medical validation through specialist diagnostic tools. If your stomach discomfort remains a constant companion for over a week, it has moved beyond simple indigestion. Recognising this persistence allows you to move toward a bespoke treatment plan, ensuring you receive the comprehensive care needed to protect your long-term digestive well-being under one roof.
Differentiating Between Acute and Chronic Gastritis Symptoms
Understanding the distinction between acute and chronic inflammation is vital for securing a faster recovery. While both conditions involve the stomach lining, their timelines and impacts on your long-term health differ significantly. Acute gastritis is essentially a sudden, severe onset of inflammation. It often feels like a temporary crisis within the digestive tract, whereas chronic gastritis acts as a persistent, low-level irritation that can last for years. Correctly identifying your specific gastritis symptoms allows our specialists to tailor a bespoke treatment plan that addresses the root cause rather than just the surface discomfort.
Sudden Onset: The Hallmarks of Acute Gastritis
Acute gastritis often arrives with little warning. It manifests as intense nausea and sharp, localized pain in the upper belly that can be quite distressing. In Singapore’s fast-paced environment, common triggers include the frequent use of non-steroidal anti-inflammatory drugs (NSAIDs) for pain relief, excessive alcohol consumption, or severe physiological stress. Some western studies indicate that acute gastritis affects approximately 8 out of every 1,000 people, showing just how common these sudden flare-ups are. When managed promptly through professional intervention and the removal of the irritant, these symptoms of gastritis typically resolve within a few days to a week. The goal is to settle the inflammation quickly to prevent any lasting damage to the gastric mucosa.
The Silent Progression of Chronic Gastritis
Chronic gastritis is a “slow burn” that develops gradually. Many patients don’t realize they have chronic inflammation until it is discovered during a routine screening or a gastroscopy for unrelated issues. A primary driver of this silent progression is the Helicobacter pylori (H. pylori) bacteria. This infection often drives chronic symptoms without causing immediate, sharp pain, allowing it to persist for decades. Over time, this ongoing irritation can lead to mucosal atrophy, where the stomach lining thins and undergoes structural changes.
We also recognize that your metabolic health plays a significant role in how your body manages inflammation. A high-performance digestive system relies on a balanced inflammatory response; when your metabolic baseline is compromised, the stomach lining may become more susceptible to chronic damage. If left unaddressed, both types can lead to erosive gastritis, a condition where the protective lining is physically worn away. This increases the risk of ulcers and internal bleeding. At our centre, we provide comprehensive diagnostic programs to help you identify these silent risks early, ensuring you gain health with minimal downtime. By addressing the inflammation before it progresses, we help you maintain a robust and pain-free digestive system.
When Gastric Pain Becomes Serious: Red Flag Warning Signs
While many people in Singapore tolerate a dull ache as a part of life, certain gastritis symptoms signal a need for immediate specialist intervention. These “red flags” suggest that the inflammation is no longer superficial but has begun to damage the structural integrity of the stomach wall. Ignoring these signs can lead to complications that are far more difficult to manage than the initial inflammation. Taking action now is the most effective way to ensure a faster recovery and prevent long-term damage.
One of the most critical signs is the appearance of black, tarry stools, medically known as melena. This occurs when blood from the upper digestive tract reacts with stomach acid, changing its colour and consistency. It’s a clear indicator of internal bleeding that requires urgent attention. Similarly, unexplained weight loss is a significant marker for concern. When chronic inflammation disrupts digestion or makes eating painful, the body lacks the fuel it needs; this often points to a more severe underlying issue than standard indigestion.
Persistent inflammation also interferes with the body’s ability to absorb essential nutrients. Chronic blood loss from an irritated lining can lead to iron-deficiency anaemia. If you find yourself feeling chronically fatigued, short of breath, or unusually pale, your stomach lining may be the culprit. At our centre, we focus on identifying these systemic impacts early to help you gain health through a bespoke, integrated approach.
Complications: From Inflammation to Ulcers
Untreated gastritis doesn’t just stay stagnant. It often progresses into peptic ulcers, which are painful open sores on the stomach lining. There is also a well-documented relationship between long-term H. pylori infection and an increased risk of gastric cancer. Professional Treatment of gastritis and regular diagnostic screening are essential to stop this progression. If you’re unsure whether your persistent discomfort has crossed into ulcer territory, understanding the key differences between stomach ulcer symptoms and acute gastritis can help you make a more informed decision about seeking specialist care. By catching changes in the mucosa early, we can implement strategies that provide less pain and shorter downtime.
A Self-Assessment Checklist for Patients
Monitoring your own health is the first step toward a pain-free digestive system. Use this framework to evaluate your risk level and determine if you need a fast-track investigation:
- Has your stomach pain or discomfort lasted for more than 7 days?
- Is the burning sensation affecting your ability to sleep through the night?
- Have you noticed any dark or tarry changes in your stool consistency?
- Are you experiencing a persistent loss of appetite or clothes feeling looser without trying?
- Do you feel unusually weak or tired despite getting enough rest?
If you answer yes to more than two of these questions, it’s time to move beyond general practitioner services and seek a specialist consultation. Early detection is the key to a faster recovery and ensures your digestive needs are handled with professional speed. We provide all your diagnostic needs under one roof to make your path to wellness as frictionless as possible.
Professional Diagnosis: The Role of Gastroscopy
When persistent gastritis symptoms don’t resolve with basic lifestyle changes, a professional diagnosis is the next logical step to ensure your long-term well-being. While many patients feel anxious about invasive tests, a gastroscopy remains the gold standard for identifying the exact state of your stomach mucosa. This procedure isn’t just about looking; it’s a fast-track diagnostic tool that provides immediate clarity. By visualising the inflammation directly, we can move away from guesswork and toward a bespoke treatment plan that guarantees a faster recovery.
For those whose primary concern is a bacterial infection, the H. pylori breath test offers a non-invasive alternative for specific cases. It’s a simple, effective way to detect the presence of bacteria without a full procedure. However, for a comprehensive view of mucosal changes or to rule out erosive damage, modern endoscopy is unmatched. We use light sedation to ensure the experience is entirely painless and comfortable. Most patients find the process much easier than they anticipated, often waking up with no memory of the procedure itself. We promise less pain and a supportive environment where your physical comfort is our primary objective.
What to Expect During a Gastroscopy
The process is streamlined for your comfort and efficiency. After a short period of fasting, the procedure itself takes only 15 to 20 minutes. During this time, the specialist can take a tiny biopsy for definitive mucosal analysis. This is crucial for distinguishing between simple inflammation and more complex cellular changes. Recovery is equally efficient. Because we prioritise less pain and shorter downtime, most patients return to their normal activities the very next day. You don’t have to put your life on hold to gain health.
Advanced Diagnostic Tools at Digestive Centre
We utilise high-definition imaging to detect early inflammatory changes that might be missed by standard equipment. This precision allows us to see the “how” and “why” of your condition with incredible detail. We also recognise that digestive issues don’t exist in a vacuum. Metabolic testing can complement these diagnostics to provide a holistic view of your overall wellness. By keeping all your digestive needs under one roof, we ensure your path from consultation to recovery is handled with professional speed and minimal administrative friction. If you’re ready to move toward a pain-free life, book a fast-track diagnostic session with our specialists today.
Managing Gastritis for Long-term Recovery
Long-term recovery from gastritis requires a strategic shift from simply masking discomfort to addressing the root cause of the inflammation. While over-the-counter antacids provide immediate, temporary relief by neutralising stomach acid, they don’t heal the underlying mucosal damage. Professional management often involves a structured course of generic medications, such as proton pump inhibitors (PPIs). These medications work by significantly reducing acid production, allowing the stomach lining the necessary environment to repair itself. When you effectively manage your gastritis symptoms through a specialist-led program, you’re not just avoiding pain; you’re actively gaining health and preventing future complications.
Dietary Adjustments and Lifestyle Changes
Effective management goes far beyond the generic advice to “avoid spicy food.” We focus on evidence-based triggers that vary from person to person. For many in Singapore, excessive alcohol consumption and highly acidic foods are primary irritants that prolong inflammation. Instead of three large meals, we recommend consuming smaller, more frequent portions. This approach reduces the total acid load on the stomach at any given time, preventing the “burning” sensation often felt after heavy dining.
Your metabolic health and weight also play a crucial role in gastric recovery. Excess abdominal weight increases intra-abdominal pressure, which can exacerbate gastric reflux and put additional strain on the stomach lining. By integrating metabolic testing with nutritional counselling, we help you identify personal dietary triggers and manage your weight effectively. This holistic approach ensures that your digestive system isn’t just surviving, but thriving.
The Specialist Advantage: Personalised Care
Relying solely on self-medication often leads to a cycle of recurring flare-ups. A bespoke treatment plan is superior because it accounts for your unique physiological profile. At Digestive Centre, we provide integrated care that brings together surgery, nutrition, and metabolic support under one roof. This comprehensive model ensures that every factor contributing to your gastritis symptoms is addressed simultaneously.
Whether you require a specific 14-day course of bismuth quadruple therapy for bacterial eradication or long-term nutritional guidance, our modern specialist approach prioritises precision. We promise less pain, shorter downtime, and a faster recovery so you can return to your daily routine. If you’re ready to move past temporary fixes and achieve lasting digestive wellness, contact Digestive Centre to schedule your fast-track diagnostic consultation.
Take Charge of Your Digestive Health
Understanding the nuances of gastritis symptoms is the first step toward regaining your quality of life. We’ve explored how to distinguish persistent inflammation from temporary indigestion and identified the red flags that require immediate specialist attention. Whether you’re dealing with a sudden acute flare-up or the silent progression of a chronic condition, early intervention remains the most effective way to prevent complications like ulcers or anaemia.
At Digestive Centre, we provide all your digestive needs under one roof. Led by Senior Consultant Surgeon Dr. Shanker Pasupathy, our fast-track diagnostic programs are designed for speed and precision. We prioritise your physical comfort with modern, painless endoscopy techniques that promise less pain and shorter downtime. Don’t let stomach discomfort hold you back from the life you deserve. Book Your Specialist Gastroscopy Consultation Today to begin your journey toward a pain-free recovery. It’s time to stop managing pain and start gaining health with a partner you can trust.
Frequently Asked Questions
Is gastritis the same as acid reflux (GERD)?
No, gastritis and acid reflux are distinct medical conditions. Gastritis is the specific inflammation of the stomach lining, whereas acid reflux occurs when stomach acid flows backward into the esophagus. While both can cause upper abdominal discomfort, their long-term impact on your digestive health differs. We provide comprehensive diagnostics for both conditions under one roof to ensure you receive the correct treatment plan for your specific needs.
Can gastritis go away on its own without treatment?
Mild cases of acute gastritis may resolve if you immediately remove the irritant, such as alcohol or specific pain medications. However, chronic inflammation rarely disappears without professional intervention and often leads to more severe complications like ulcers. Ignoring persistent gastritis symptoms can result in long-term mucosal damage, so seeking a specialist consultation is the most reliable way to ensure a fast-track recovery and gain health.
How long does it take for gastritis symptoms to clear up?
Acute symptoms typically begin to improve within 3 to 7 days once the underlying cause is addressed and treatment starts. Chronic gastritis requires a more prolonged approach, often taking several weeks or even months of consistent medication and dietary changes to achieve full mucosal healing. Our goal is always to provide less pain and shorter downtime through a bespoke management plan tailored to your recovery speed.
Is gastritis a contagious condition?
Gastritis itself isn’t contagious, but the H. pylori bacteria that frequently causes it can be transmitted through saliva or contaminated food and water. In Singapore, it’s common for family members to share the infection, which is why we may recommend screening for those living in the same household. Eradicating the bacteria is a critical step in stopping the spread and protecting your family’s long-term digestive wellness.
What is the most common cause of gastritis in Singapore?
The most frequent drivers of stomach inflammation in Singapore are H. pylori bacterial infections and the frequent use of non-steroidal anti-inflammatory drugs (NSAIDs) for pain relief. Lifestyle factors, such as high alcohol intake and the consumption of extremely spicy or acidic foods, also play a significant role in triggering flare-ups. Identifying your specific cause through a professional gastroscopy allows us to create an integrated and effective healing strategy.
Can stress alone cause gastritis symptoms?
Emotional stress doesn’t directly cause the clinical inflammation of the stomach mucosa, but severe physiological stress from major trauma or surgery can lead to “stress ulcers.” While daily work stress won’t create the inflammation, it can significantly worsen your perception of gastritis symptoms and trigger more frequent flare-ups. We address these factors through holistic care that combines medical treatment with lifestyle and nutritional counselling for better outcomes.
Does a gastroscopy require an overnight hospital stay?
No, a gastroscopy is a routine day procedure in Singapore that does not require an overnight stay. The entire process, including the procedure and the necessary recovery time from sedation, usually takes about 2 to 3 hours. Most patients are able to return home shortly after the examination and resume their normal activities by the following day, ensuring minimal disruption to your busy schedule.
What should I eat during a gastritis flare-up?
Focus on bland, low-acid foods like plain porridge, steamed chicken, and non-citrus fruits like bananas during an active flare-up. It’s essential to avoid caffeine, alcohol, and oily foods that can further irritate the already inflamed stomach lining. We recommend consuming smaller, more frequent meals to reduce the acid load on your stomach, and our nutritional experts can provide a personalised plan to help you identify your unique triggers.

